Comparison between Bethesda System and Conventional System for Standardization of Reporting Thyroid Cytopathology
*Saleheen S,1 Rahman DA,2 Chowdury MA,3 Haque MM,4 Habib S,5 Khan KH6
- * Saied Saleheen, Assistant Professor, Department of Pathology, Sheikh Hasina Medical College, Tangail. saleheen44@gmail.com
- DM. Arifur Rahman, Assistant Professor, Department of Pathology, TMSS Medical College, Gokul, Bogura,
- Mehdi Ashik Chowdury, Assistant Professor, Department of Pathology, Jahurul Islam Medical College, Bajitpur, Kishoreganj.
- Mohammad Mahbubul Hoque, Lecturer, Department of Pathology, Sheikh Sayera Khatun Medical College, Gopalganj.
- Saequa Habib, Associate Professor, Department of Pathology, Bangabandhu Sheikh Mujib Medical University, Dhaka.
- Kamrul Hasan Khan, Professor, Department of Pathology, Bangabandhu Sheikh Mujib Medical University, Dhaka.
*For correspondence
Abstract
Background: Fine-needle aspiration cytology (FNAC) is considered as an effective test to screen and diagnose patients with thyroid swelling for surgical management. But FNAC still suffers because of its inherent limitations as well as variability in its diagnostic terminology.The Bethesda System of Reporting Thyroid Cytopathology (TBSRTC) may improve the state. This study was to report the experience in using this reporting system to redistribute the cytological diagnoses made by conventional system and also to evaluate the specificity, sensitivity, accuracy and predictive values as a tool to compare both the methods based on the correlation between cytopathology and histopathology.
Methods: A total of 73 patients presenting with thyroid swelling were subjected to FNAC and reporting was done according to the conventional system and TBSRTC. The cytological diagnosis was correlated with the histopathological diagnosis. The sensitivity, specificity, predictive values were calculated considering cytology as screening test.
Results: In this study, TBSRTC was found superior because of higher sensitivity (91.66%) and specificity (97.77%) as compared to conventional system (80.76% and 87.23% respectively). Positive predictive value, negative predictive value and diagnostic accuracy of Bethesda system were 95.65%, 95.65% and 90.41% respectively which were also significantly higher as compared to those of conventional system (77.78%, 89.13% and 84.93% respectively).
Conclusions: TBSRTC may improve the efficacy of thyroid FNAC as a screening test.
[Journal of Histopathology and Cytopathology, 2020 Jan; 4 (1):38-47]
Keywords: Comparison, Thyroid FNAC, Bethesda system (TBSRTC), Conventional system, Histopathology, Standardization
Introduction
Fine Needle Aspiration Cytology (FNAC) is a quick, cost-effective and minimally invasive outpatient procedure used worldwide in the initial diagnosis of thyroid swellings. As it can distinguish between benign and malignant lesions quite effectively, it is the preoperative screening method of choice worldwide.1 Before the routine use of thyroid Fine Needle Aspiration (FNA), the percentage of surgically resected thyroid nodules that were malignant was 14%.2 With current thyroid FNA practice, the percentage of resected nodules that are malignant surpasses 50%.3
However, due to the lack of a standardized system of reporting, pathologists have been using different terminologies and diagnostic criteria, leading to confusion amongst clinicians in the interpretation of the cytopathology report and ultimately hindering a definitive clinical management.4 It has also hindered the sharing of clinically meaningful data among multiple institutions.5 To mitigate this confusion all the pathologists need to use the same diagnostic criteria and terminology.6
Various reporting formats of thyroid FNAs have been suggested in the literature since the 1970s when thyroid FNAs began to be the subject of publications, and new formats continued to emerge.7 Several classification schemes have been suggested by various authors based on personal/institutional experiences but there is general support for the utilization of a tiered classification system.5 With this background, the National Cancer Institute (NCI), Bethesda, Maryland, United States, published an atlas and guidelines using standardized nomenclature for the interpretation of thyroid FNAC known as The Bethesda System for Reporting Thyroid Cytopathology (TBSRTC).4 It categorized the thyroid FNAC diagnoses into six groups with well-defined cancer risk and clear indications for further clinical management.8 It has also increased the interobserver reproducibility of cytopathological diagnoses of thyroid lesions.9-12
TBSRTC has been well received by both pathologists and clinicians and has been widely implemented by pathology laboratories in USA and in several European countries.13 Following publication of TBSRTC, the reporting system used in the United Kingdom since 2002, was updated by a working group of The Royal College of Pathologists and is now quite similar to TBSRTC.14 But TBSRTC still has to go a long way in getting acceptability in many countries of Asia and Africa.10
A good number of studies have been carried on in several countries in Asia (India, Pakistan, Iran, Korea and KSA) regarding usefulness of TBSRTC and it has been proved useful for management of patients with thyroid swelling in these countries.9,11,15-20 But this relatively recent six category scheme still needs to be validated by more prospective studies with histopathological correlation.16
In Bangladesh, there is no known reporting scheme using tiered classification system. The utility of thyroid cytopathology reporting according to TBSRTC in context of Bangladesh is also unexplored. Standardization of the reporting system by TBSRTC may result in improvement of the quality, homogenization and also reduce interobserver variability of thyroid cytopathology reports. In this context, this study was performed to assess the predictive values, sensitivity and specificity and accuracy of the TBSRTC in comparison with that of the conventional system used in the BSMMU, Dhaka, Bangladesh with histopathological correlation. The view was to observe the usefulness of Bethesda system for standardization of thyroid cytopathology reporting in the context of this country (Bangladesh).
Methods
This is a cross sectional study carried out at the Department of Pathology, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka during the period from March 2015 to February 2017. A total of 73 patients presenting with thyroid swelling were included in this study, who has undergone FNA followed by the biopsy of the thyroid lesions. Patients presenting with thyroid swelling in any lobe of thyroid detected by clinical palpation (multinodular, solitary nodule, diffuse goiter etc) were included except those unwilling to be involved into the study.
All clinical information were recorded in a pre-designed proforma including demographic features, address and telephone contacts (for histological follow up). Results of all the routine investigations with special attention to ultrasonography of neck, serum T3, T4, and TSH levels and thyroid scintigraphy were noted where available.
FNA of all patients was performed at the Department of Pathology, BSMMU. Smears were stained with Papaniculaou (PAP) and Hematoxylin and Eosin (H&E) stains. Cytological findings were recorded and diagnoses were made according to both conventional and TBSRTC for each cases. For the TBSRTC reporting the Atlas10was used as manual (Table I). Reports were issued according to conventional method.
Koss’ Diagnostic Cytology and its histopathologic bases21 was followed conventionally as reference book in this department. The diagnoses made by conventional system are mostly based on its reference. The diagnoses were: Non-neoplastic lesions: Nodular goiters (NG) including cystic degeneration (CD), Lymphocytic thyroiditis (LT), Hashimoto thyroiditis (HT), Nodular goiter with co-existent thyroiditis, Multinodular goiter (MNG).
Cellular follicular lesion (CFL): Cellular smears on cytology that included goiters with adenomatous changes, follicular adenomas and carcinomas, as well as the follicular variant of papillary carcinomas. In BSMMU suspicious cytology, atypia of undetermined significance and other gray zone cytology are also included within this diagnosis.
Neoplastic lesions: Papillary thyroid carcinoma (PTC), suggestive of papillary carcinoma, medullary thyroid carcinoma (MTC) etc.
Biopsy specimens or histopathological reports of the patients undergoing surgery following the FNA interpretation under this study were collected. The histopathological findings were correlated with cytopathological findings and were recorded accordingly.
Descriptive analytical statistics was calculated. Thyroid FNA was considered as a ‘screening test’ and histopathology as gold standard. FNA benign was considered to be negative and the remaining categories were considered to be positive because they indicated significant risk of malignancy and led to a recommendation of surgery.8 Sensitivity, specificity, accuracy, the positive predictive value (PPV) and negative predictive value (NPV) were calculated from the available data by statistical formulae. In this study, Thyroid FNA has been considered as a screening method as TBSRTC is formed by NCI as a screening method to triage the patients effectively into groups that need surgery and the other that do not.5
For calculating statistical parameters nondiagnostic (ND) and AUS/FLUS cases were excluded as non-definitive diagnoses and categories, SFM and malignant were put together in most of the studies.15,16,22-24 In this study, the inadequate/ND cases were reaspirated and have been included rationally in other categories. Those which were still inadequate, had been excluded from statistical analysis.
Results
Out of the 73 cases 62(84.9%) were female and 11(15%) were male. The age of the patients ranged from 16 to 70 years with average age around 40 years.
According to the conventional system forty five (61.64%) cases were diagnosed nodular goiter. Five (11.11%) of these lesions were found to be neoplastic (one benign and 4 malignant) on histopathology. Although all PTC and suggestive of PTC categories were found neoplastic and also malignant, 60% of the cellular follicular lesions (9 out of 15) were neoplastic (one benign and 8 malignant) and the rest were benign on final histological diagnosis.
The lesions when redistributed according to the Bethesda system: 46 (63%), 04 (5.4%), 03 (4.1%), 08 (10.95%), 12(16.4%) of the lesions were diagnosed as Cat-II, Cat-III, Cat-IV, Cat-V and Cat-VI respectively. The redistribution of the lesions after application of Bethesda system is shown in Table-II.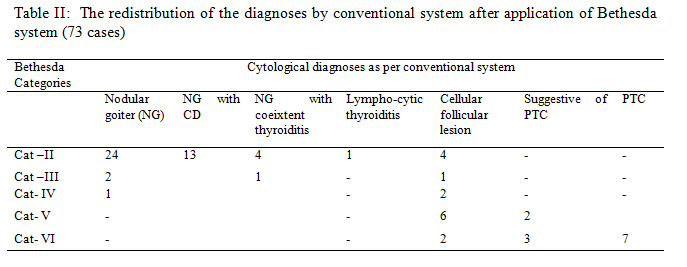
Out of 73 cases, 64 (22 neoplastic and 42 non-neoplastic) cytological diagnoses were concordant on both the conventional and Bethesda systems. One lesion was non-neoplastic on conventional but diagnosed neoplastic on Bethesda system while 04 neoplastic lesions by conventional system were categorized as non-neoplastic by Bethesda system. Three non-neoplastic and one neoplastic case according to conventional system were categorized as Cat- III (AUS) by Bethesda system. The CFL on conventional system were distributed by the Bethesda system into various categories that matched well (Table-III) with final histological diagnoses.


All the neoplastic lesions irrespective of benign and malignant neoplasm were considered positive for both the histological and cytological diagnoses, as they recommend for surgical excision. The concordances of the cytological diagnoses made by two methods with the final histological diagnoses are shown in Table IV.
Granulomatous thyroiditis: GT, Follicular adenoma: FA, Follicular carcinoma: FC, FVPTC: Follicular Variant of PTC, WDTUMP: Well differentiated tumor of uncertain malignant potential.
Diagnoses made according to TBSRTC shows increased overall concordance with hisotoathological diagnosis than that of the conventional system.
FNA interpretation by conventional method yielded significant false positive (6) and false negative (5) diagnoses. While analyzing the smears by the Bethesda system had decreased both the false positive (1) and false negative (2) interpretations. The sensitivity, specificity, accuracy and predictive values calculated for both the methods by using the statistical formulas are compared to each other in the Table V. 
Sensitivity and positive predictive value (PPV) of the Bethesda system were found better (91.66% and 95.65% respectively) when compared to that the conventional system (80.76% and 77.78% respectively). The specificity and negative predictive values (NPV) were also found higher for Bethesda system (97.77% and 95.65%) in comparison to that of the conventional system (87.23% and 89.13% respectively). Diagnoses according to the Bethesda categories were 90.41% accurate where accuracy for the conventional system was 84.93%.
Discussion
Reporting according to the conventional system included 41 (about 56.16%) patients into benign category, while category-II (Benign) in the Bethesda system included 44 (60.27%) patients. All (12) the suspicious for malignancy and malignant diagnoses on conventional system corresponded to category V and VI of Bethesda system. It reflects that there was actually no significant change in diagnosis of unequivocally benign and malignant cases according to the two systems of reporting.
15 (20.54%) CFL diagnosed by conventional system was the major field where the Bethesda system varied markedly. So, CFL was a “gray zone” diagnosis that included some benign (26.67%) and malignant (53.33%) cases.25 These cases when reclassified by the Bethesda system yielded more specific results with good histological correlation (Table IV). This difference can be explained by- i) Subjective underscoring of some neoplastic cytologies which are of SFM category in more objective Bethesda system and ii) Assigning the follicular lesion diagnosis for some hyper cellular smears of goiter arranged in folded sheet appearance.
The 06 false-positive FNA diagnoses in conventional system included cellular smears of histologically nodular goiters that were interpreted as CFLs. Four of these cases were interpreted benign (category-II) by Bethesda system and 01 case was designated category-IV (suspicious for Hurthle cell neoplasm) because of relative abundance of Hurthle cells showing pleomorphism. Five cases were false negative for conventional method, 04 of which were due to compromised cytology samples. The rest one case diagnosed conventionally as nodular goiter that was histologically follicular adenoma and Category-IV (SFM) in Bethesda system.
When compared with other studies using TBSRTC with histological follow up, sensitivity and NPV of the present study were consistent with most of the studies (Table VI). The specificity and PPV were higher than most of the other studies, which may be due to small sample size in this present study.
Conclusion
By dint of its higher sensitivity, specificity, predictive values and accuracy TBSRTC has been proved to be better than conventional system for reporting thyroid cytopathology. So, it should be useful for standardization of thyroid cytopathology reporting. However, studies needed to explore its effect in reducing inter-observer variation of reporting thyroid cytopathology as well as its usefulness to the clinicians in decision making.
References
- Bagga PK, Mahajan NC. Fine needle aspiration cytology of thyroid swellings: How useful and accurate is it? Indian Journal of cancer, 2010 Oct 1;47(4):437.
- Hamberger B, Gharib H, Melton LJ, Goellner JR, Zinsmeister AR. Fine-needle aspiration biopsy of thyroid nodules: impact on thyroid practice and cost of care. The American journal of medicine. 1982 Sep 1;73(3):381-4.
- Yassa L, Cibas ES, Benson CB, Frates MC, Doubilet PM, Gawande AA et al. Long‐term assessment of a multidisciplinary approach to thyroid nodule diagnostic evaluation. Cancer Cytopathology: Interdisciplinary International Journal of the American Cancer Society. 2007 Dec 25;111(6):508-16.
- Mondal SK, Sinha S, Basak B, Roy DN, Sinha SK. The Bethesda system for reporting thyroid fine needle aspirates: a cytologic study with histologic follow-up.Journal of Cytology. 2013; 30(2):94.
- Cibas ES, Ali SZ. The Bethesda system for reporting thyroid cytopathology. Thyroid. 2009 Nov 1;19(11):1159-65.
- Schinstine M. Pathology Hawaii Hotline: A Brief Description of the Bethesda System for Reporting Thyroid Fine Needle Aspirates. Hawaii medical journal. 2010 Jul; 69(7):176.
- Wang HH. Reporting thyroid fine‐needle aspiration: literature review and a proposal. Diagnostic cytopathology. 2006 Jan; 34(1):67-76.
- Ali SZ and Cibas ESThe Bethesda system for reporting thyroid cytopathology: definitions, criteria and explanatory notes. Springer Science & Business Media.2010
- Ahmed S, Ahmad M, Khan MA, Kazi F, Noreen F, Nawaz S, Sohail I. The interobserver reproducibility of thyroid cytopathology using Bethesda Reporting System: Analysis of 200 cases. J Pak Med Assoc. 2013 Oct 1;63(10):1252-5.
- Bhasin TS, Mannan R, Manjari M, Mehra M, Sekhon AK, Chandey M, Sharma S, Kaur P. Reproducibility of ‘The Bethesda System for reporting Thyroid Cytopathology’: a multicenter study with review of the literature. Journal of clinical and diagnostic research: JCDR. 2013 Jun; 7(6):1051.
- Mufti ST, Molah R. The Bethesda system for reporting thyroid cytopathology: a five-year retrospective review of one center experience. International journal of health sciences. 2012 Jun; 6(2):159.
- Pathak P, Srivastava R, Singh N, Arora VK, Bhatia A. Implementation of the Bethesda System for Reporting Thyroid Cytopathology: interobserver concordance and reclassification of previously inconclusive aspirates. Diagnostic cytopathology. 2014 Nov; 42(11):944-9.
- Auger M, Nayar R, Khalbuss WE, Barkan GA, Benedict CC, Tambouret R et al. Implementation of the Bethesda System for Reporting Thyroid Cytopathology: observations from the 2011 thyroid supplemental questionnaire of the College of American Pathologists. Archives of Pathology and Laboratory Medicine. 2013 Nov; 137(11):1555-9.
- Crippa S, Dina R. Interobserver reproducibility of thyroid fine-needle aspiration using the UK Royal College of Pathologists’ classification system. American journal of clinical pathology. 2012 May 1;137(5):833-5.
- Mamatha M, Sekhar SC, Rani HS, Anil SS and Vandana G. A comparative study between conventional system and the Bethesda system applied for reporting thyroid cytopathology. International Archives of Integrated Medicine.2015; 2(3):87 – 95
- Mehra P, Verma AK. Thyroid cytopathology reporting by the Bethesda system: a two-year prospective study in an academic institution. Pathology research international. 2015;2015. 240505.doi: 1155/2015/240505
- Ahmed S, Ahmad M, Khan MA, Kazi F, Noreen F, Nawaz S, Sohail I. The interobserver reproducibility of thyroid cytopathology using Bethesda Reporting System: Analysis of 200 cases. J Pak Med Assoc. 2013 Oct 1; 63(10):1252-5.
- Bukhari MH, Khan AA, Niazi S, Arshad M, Akhtar ZM, Al-Sindi KA. Better thyroid cytopathology reporting system may increase the clinical management and patients outcome. J Cytol Histol. 2012;3(6):1000158.
- Hajmanoochehri F, Rabiee E. FNAC accuracy in diagnosis of thyroid neoplasms considering all diagnostic categories of the Bethesda reporting system: A single-institute experience. Journal of Cytology/Indian Academy of Cytologists. 2015 Oct; 32(4):238.
- Jo VY, Stelow EB, Dustin SM, Hanley KZ. Malignancy risk for fine-needle aspiration of thyroid lesions according to the Bethesda System for Reporting Thyroid Cytopathology. American journal of clinical pathology. 2010 Sep 1;134(3):450-6.
- Sanchez AM and Stahl RE.The Thyroid, Parathyroid, and Neck Masses Other Than Lymph Nodes.in: Koss LG, Melamed MR, editors. Koss’ diagnostic cytology and its histopathologic bases. Lippincott Williams & Wilkins; 2006.pp1148-1173.
- Joshi D and Jesalpura NS. Comparision Between Bethesda System and Conventional System in Thyroid Cytopathology: International Journal of Scientific Research, 2015;4(9).
- Naz S, Hashmi AA, Faridi N, Edhi MM, Kamal A and Khan M. Diagnostic accuracy of Bethesda system for reporting thyroid cytopathology: an institutional perspective.International archives of medicine, 2014; 7(1):46..
- Theoharis CG, Schofield KM, Hammers L, Udelsman R, Chhieng DC. The Bethesda thyroid fine-needle aspiration classification system: year 1 at an academic institution. Thyroid. 2009 Nov 1;19(11):1215-23.
- Bonzanini M, Amadori P, Morelli L, Fasanella S, Pertile R, Mattiuzzi A et al. Subclassification of the “grey zone” of thyroid cytology; a retrospective descriptive study with clinical, cytological, and histological correlation. Journal of thyroid research. 2011:251680.doi:10.4061/2011/251680.
- Gupta M, Gupta S, Gupta VB. Correlation of fine needle aspiration cytology with histopathology in the diagnosis of solitary thyroid nodule. Journal of thyroid research. 2010 Apr 18;2010:379051.


