Present Status of Cervical Cancer Screening in Bangladesh
*Nessa A,1 Khanom Q,2 Ripa SZ,3 Khan KH,4 Azad AK,5 Kamal M6
Abstract
| Cervical cancer is the second-most common cancer among women in Bangladesh. The Government of Bangladesh (GOB) has introduced a cervical cancer screening programme through Visual Inspection of Cervix with Acetic Acid (VIA). After a pilot programme in 16 districs out of 64 in 2005, VIA facilities have graduallybeen scaledup to the remaining 48 districts and to half of the sub-districts (Upazilas). Till date, 2212 service providers (408 doctors and 1904 nurses, family welfare visitors, paramedics) of 431 VIA centres received training and are offering VIA to women aged 30 years and above. After establishing the VIA centre at each selected Upazila, a three to four-day long VIA camp is being organized with facilities of awareness creation and screening. Since 2005, 188 doctors/ nurses received training on colposcopy, 43 Pathologists and 57 Medical Technologist from BSMMU and different MCHs were trained on histopathology. Screen positive cases are referred to the colposcopy clinics of tertiary level health-care facilities (BSMMU/15 Medical College Hospitals) for evaluation and management. From January 2005 to June 2018, 2012752 VIA tests were performed at different facilities throughout the country; among the tested women, 92037 (4.5%) were found VIA-positive. Among the women with VIA-positive report, 26773(29.1%) attended the colposcopy clinic of BSMMU,of which 11501(44.0%) had precancerous and 1897 (7.0%) had cancerous conditions of the cervix.3563 (13.30%) were treated by local excision (LEEP, Loop Electrosurgical Excision Procedure), 2781 (10.40%) by local ablative method (thermal ablation) and1646 (6.15%) women with cervical cancer were referred to oncology. |
[Journal of Histopathology and Cytopathology, 2019 Jan; 3 (1):45-52]
Keywords: Cervical, Cancer, Screening, VIA, Bangladesh
Introduction
Cervical cancer (CC) is the fourth most common cancer among women worldwide with an estimated 569,847 new cases and 311,365 deaths in the year 2018.In Bangladesh, the incidence of CC was 8068 and CC constitutes about 12% of the female cancer in this country.1 Survival of cancer patients is strongly determined by stage at diagnosis. The overall 5-year relative survival for early and localized cancers is 73.2%, but can be as low as 7.4% for advanced stage disease.2 Due to the late stage at diagnosis and inadequate management facilities, mortality rate from CC is still high in Bangladesh. Successful screening program is, therefore, one of the effective ways for early diagnosis and prevention of this cancer. All the tertiary level hospitals and institutes of this country are carrying a large load of CC patients. Treatment of this cancer is expensive and requires radical operative procedures, prolonged hospital stay, and/or radiotherapy/ chemotherapy. In Bangladesh, facilities for radiotherapy are available only in few institutions and expensive in the private sector.
- *Dr. Ashrafun Nessa, Professor, Department of Gynaecological Oncology, Bangabandhu Sheikh Mujib Medical University (BSMMU), Shahbag, Dhaka, Bangladesh.
- Quayuma Khanom, Colposcopist, Department of Obstetrics and Gynaecology, BSMMU.
- Sadia Zaman Ripa, Colposcopist, Department of Obstetrics and Gynaecology, BSMMU
- Professor Dr. Kamrul Hasan Khan, Professor, Department of Pathology, BSMMU.
- Professor Dr Abul Kalam Azad, Director General, Directorate General of Health Services, Mohakhali, Dhaka, Bangladesh.
- Professor Dr. Mohammed Kamal, Professor, Department of Pathology, BSMMU.
*For correspondence
Development of CC Screening Programme
Government of Bangladesh (GOB) adopted VIA (Visual Inspection of Cervix with Acetic Acid) method for CC screening due to its simplicity, low cost, potential for immediate linkage with investigations/treatment and the possibility of rapid training to the service providers. A pilot programme evaluated the feasibility of screening with VIA within the existing government health infrastructure in 16 districts during 2005.3-5 Thereafter GOB gradually scaled up the programme by 2010 towards the district level of all districts with support from BSMMU and UNFPA.
Since 2012, GOB and BSMMU initiated timely intervention through a development of project “Establishment of National Centre for Cervical and Breast Cancer Screening and Training at BSMMU” (2012-2018). Through this project a ‘National Centre for Cervical and Breast Cancer Screening and Training (NCCBCST) at BSMMU, has been established by MOHFW for rapid development of competency-based training for service providers from different levels of health care, better coordination, scale up of the programme and improvement of the screening coverage. Through the project ‘Cervical and Breast Cancer Screening Programme’ was scaled up towards 180 Upazilas to provide facilities towards grass root level.
According to WHO regional policy framework, cervical cancer screening policy should be organized cancer screening programme.6 Therefore, since June 2018, GOB and BSMMU initiated another Development project “Electronic Data Tracking with Population-based Cervical and Breast Cancer Screening Programme (2018-2021)”. A population-based, organized cancer screening programme should be managed through the public health delivery system and follow a uniform guideline, achieve a reasonable coverage of the target population and have efficient linkage between screening and treatment of the positive cases. Through this project such a population-based cervical and breast cancer screening programme is being initiated from community with a good referral linkage to secondary and tertiary level health care system along with rapid development of services from different health care system, better coordination and scale up of the programme to improve the screening coverage.
Screening Facilities
The screening programme is being implemented through capacity building of service providers such as Senior Staff Nurses (SSN), Family Welfare Visitors (FWVs) and doctors/Gynaecologists from Institutes/ MCHs through training on VIA and clinical breast examination (CBE) from 64 districts. VIA is performed at Medical College Hospitals (MCHs), BSMMU, District Hospitals (DHs), Maternal and Child Welfare Centres (MCWCs), selected Upazila Health Complexes (UHCs), few NGO clinics by trained FWVs, Paramedics, SSNs, and Doctors.3-5, 7-10
Till now, about 431 VIA and CBE facilities has already been established at primary, secondary and tertiary level health care facilities of 64 districts of Bangladesh (Table I). The GOB introduced screening services free of cost for all women of 30-60 years in all districts of Bangladesh.
Table I: Total number of VIA and CBE centers
| Name of Locations | Number of Centers |
| District Hospitals | 15 |
| BSMMU, NICRH, ICMH MCHs | 57 |
| MCHTI, MFSTC, MCWC | 61 |
| UHCs | 248 out of 488 |
| Union Health & Family Welfare Centres | 30 out of 3725 |
| BGB,CMH/ Private/NGOs | 20 |
| Total= | 431 |
CBE= Clinical Breast Examination
MCHTI =Maternal and Child Health Training Institute
MFSTC= Mohammadpur Fertility Services & Training Centre
UHC= Upazila Health Complexes
BGB= Border Guard, Bangladesh Hospital
The target population and frequency of screening
WHO recommends screening from 30 years of age, with population screening coverage of women aged 30 to 49 years of age.11,12 Best utilization of the resources is possible if screening is limited to this age group with maximum possibility of detecting the high grade precancer lesions (CIN II and III). Individual countries may adopt variations depending on the government’s attitude and political will, stakeholder’s view, economic situation, the budgetary allocation etc. GOB has taken a policy for not to screen women prior to 30 years of age. Moreover, screening women at a younger age detects many low-grade lesions that are self-limiting and do not usually progress into cancer. However, GOB is adopting a policy to screen women of 30-60 years of age. The screening will be performed every five years. All efforts should be made to achieve a good coverage of the target population within next five years.
Record-keeping and Data Management
Maintenance of records, storage of data related to various components of screening, and periodic reports are essential for an organized screening programme. For population based organized screening, countries need to develop an electronic database for all women of target age. The GOB initiated development of database with women’s basic information, screening, colposcopy, treatment and follow up records. The computerized database will be maintained at each screening centre and all colposcopy centres. A mechanism to check the compliance of screen-positive women to colposcopy and/or treatment should be established by the government.
Performances of the Screening Programme
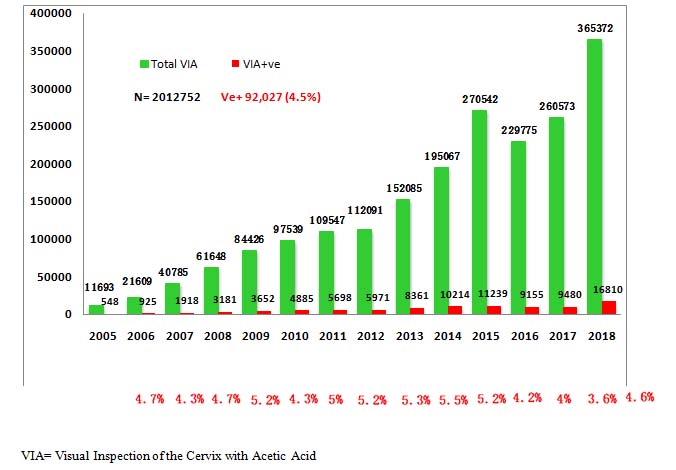
From January 2005 to December 2018, 2012752VIA tests were performed at different facilities; among the tested women, 92037 (4.5%)were found VIA-positive. The coverage of the screening tests is increasing every year (Fig 1).
Fig 1: Number of VIA tests and VIA+ve results (2005 to 2018)
(Total= 2012752, Positive 92,027 (4.5%)
VIA= Visual Inspection of the Cervix with Acetic Acid
Evaluation and Management of Screen Positive Cases
Women with VIA-Negative reports are advised to have repeat test after 5 years and screen positive cases are being referred to the colposcopy clinics of tertiary care facilities (BSMMU/ MCHs), where evaluation and management are carried out.5, 7-10 14 government MCHs and BSMMU are functioning as referral centres through development of colposcopy clinics. All women have colposcopic examination by experienced colposcopists using standard colposcopes after oral consent.
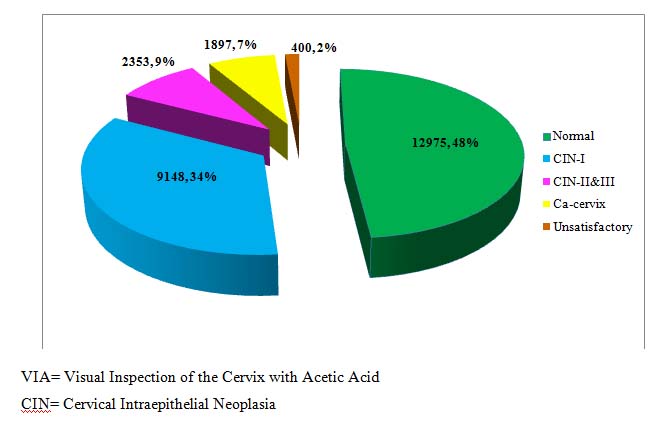
Among the VIA positive women throughout the country, 26773(29.1%) attended the colposcopy clinic of BSMMU of which 11501(44.0%) had colposcopy diagnosed precancerous and 1897 (7.0%) had cervical cancer (Fig 2).
VIA= Visual Inspection of the Cervix with Acetic Acid
CIN= Cervical Intraepithelial Neoplasia
Fig 2. Colposcopy Findings of VIA-positve Women Attending BSMMU (January 2005 to December 2018, N= 26773)
All colposcopy diagnosed pre-cancer cases are offered treatment and the results of the biopsies should also be recorded in the colposcopy registry books. Cervical pre-cancers are treated either by removing the entire abnormal area with or with destruction of abnormal tissue. Among the 26773 attending women at BSMMU, 3563 (13.30%) were treated by local excision (LEEP, Loop Electrosurgical Excision Procedure), 2781 (10.40%) by local ablative method (thermal ablation).Women with CC (N=1646, 6.15%) were referred to the Department of Oncology of BSMMU, NICRH and other institutes for further management(Table II). All LEEP specimen and specimen collected by punch biopsy forceps before treatment were sent for histological examination.
Table II: Management of Referred Patients at BSMMU (January 2005 to December 2018)
| Management of Women | Number |
| Follow-up after 3 years | 12161 (45.40%) |
| Follow-up after 1 year | 3544 (13.25%) |
| LEEP | 3563 (13.30%) |
| Cryotherapy | 131 (0.50%) |
| Thermal Ablation | 2781 (10.40%) |
| Referred to Oncology due to Cancer | 1646 (6.15%) |
| Failure of treatment and follow-up | 2947 (11.00%) |
| Total | 26773 (100.00%) |
LEEP = Loop Electrosurgical Excision Procedure
To improve performance of the cervical and breast pre-cancer and cancer diagnosis, 43 Pathologists from BSMMU and different MCHs were trained with the support of Pathology specialist of Department of Cytology & Gynae, Postgraduate Institute of Medical Education & Research, Chandigarh, India. Trainer from International Agency for Research on Cancer (IARC) strengthen the training of 57 Histopathology technician from different MCHs on cervical & breast pre-cancer diagnosis.
In Bangladesh, the excision method, Loop Electrosurgical Excision Procedure (LEEP) has acquired acceptability as a commonly used treatment method for cervical pre-cancers and performed as an outpatient procedure under local anaesthesia.3,4,7,8 Among the ablative methods, thermo-coagulationis a safe, simple and effective ablative technique to treat selected cervical pre-cancers. In Bangladesh Thermo-coagulation has been generously used recently at several tertiary health facilities and at health camps of many UHCs.8,9 Facilities for LEEP are available at BSMMU and about 15 Government MCH and the facilities of thermo-coagulation is available at BSMMU and 6 selected MCHs free of cost.
Ensuring management of the screen-positive women
All screen-positive women should have adequate counselling, evaluation and treatment at appropriate facilities. In Bangladesh, women with VIA positive report have evaluation using colposcopy through addition of a second visit at a higher referral system and women with suspected CIN of any grade should have treatment at the same visit without any histopathological confirmation of the disease. This strategy is called ‘see and treat’ or ‘colposcopy and treat’ approach. This approach is convenient for the woman,reduces her anxiety, improves compliance to treatment, and is cost-effective. In Bangladesh, ‘see-and-treat’ approach for high grade diseases combining colposcopy and LEEP/ thermal ablationhas been adopted since the year 2010 to improve compliance oftreatment.7,9
Follow-up of treated patients should be continued at all level of facilities by available methods. VIA, colposcopy, Pap smear or HPV DNA test can be used during follow-up on an annual basis for three years. Women tested negative on three consecutive rounds should be returned to the routine screening protocol applicable to the normal population.
National Strategy for CC Prevention & Control (2017-2022)13
National Strategy for CC Prevention & Control (2017-2022)in Bangladesh was developed by DGHS and approved by MOHFW.This strategy developed a broad guidelines to strengthen the National CC Control Programme byintroducingvaccination programme for adolescent girls against the Human Papillomavirus (HPV) through Expanded Program on Immunization(EPI) and implementing population based organized CC screening and treatment through public delivery system. GOB planned to implement organized population-based CCscreening programme to achieve a reasonable coverage of the target population.Married womenbetween 30-60 years of age is offered VIA-basedscreening at an interval of 5 years. All screen-positive women shouldbe evaluated by colposcope/mini-colposcope and treated at appropriatefacilities. All grades of colposcopy suspected cervical pre-cancers shall be treated following “see andtreat strategy” during the same visit if applicable. Adequate human resources,strengthening of relatedhealth infrastructure, electronic datamanagement will be organized.Institution Heads and Gynaecology consultants of all level of health care system shouldbe responsible for implementation, coordination of servicedelivery and quality assurance of the programme. Common performance indicators are coverage of the target population, screening test positivity, compliance to treatment and detection rates of CIN-II, or worse disease.Outcome indicators should be monitored on a regular basis to identify gaps and to identify ways of improvement.
Detection of early cervical cancer, facilities for staging and diagnostic workup, appropriate treatment based on stage of the disease will be ensured. Gynaecologists, gynaecologic oncologists, histopathologistsshould be made available at all tertiary care centers for surgical management of early-stage cancers. Radiation therapy and chemotherapy facilities should be made available at selected tertiary care hospitals, including dedicated oncology centers.The capacity of health systems should be improved to ensure the treatment of cancer patients on time. An appropriate evaluation and treatment services for pre-invasive and invasive cervical cancers such as colposcopy, thermo-coagulation, LEEP, radical surgery, radiation-therapy/chemo-therapy, alone or in combination should be established. The concept of palliative care to policy-makers, health-care planners, administrators, and the general people should be promoted. An inter-professional team including doctor, nurse, social worker, counselor need to be developed to deliver the palliative care services. Availability of essential drugs for the management of pain and other symptoms including access to an adequate and uninterrupted supply of oral morphine at all facilitiesshould be ensured.
Discussions
The prevalence of CC is high in Bangladesh and large numbers of women have precancerous condition of the cervix. The GOB is taking active steps to improve screening services up to the grass root level. Till now most of the districts of Bangladesh have at least six centres for CC screening. The programme is providing opportunistic screening services presently, GOB has already initiated development oforganized population based screening services with positive expectation of reducing CC.
In Bangladesh, with expansion of the programme, gradually increasing number of women will need evaluation and treatment for cervical pre-cancer. Treatment by LEEP may not be feasible for large scale practice due to expensive equipments, lack of trained personnel and possible complications. Cryotherapy though is an effective method of treatment, it requires refrigerant gases which is not widely available in Bangladesh and transport cost is high. Therefore, the small, light, comparatively cheap and readily portable thermocoagulator operated by electricitybecame a feasible alternative to cryotherapy.It can be used generously for treatment of cervical pre-cancer at all level of health care system. Health care providers can be rapidly trained in using thermo coagulator and its maintenance.
Conclusion
The ultimate goal of the programme is to reduce cervical cancer prevalence through treatment of cervical pre-cancer in this country. Almost all cases of cervical cancer are caused by certain strains of human papilloma virus (HPV). It is also revealed that different socio-demographic and reproductive factors have association with cervical cancer. Research should alsofocus to evaluate the influence of different demographic and reproductive risk factors for developing cervical pre-cancer and cancer.
References
- Ferlay J, Ervik M, Lam F, Colombet M, Mery L, Piñeros M, Znaor A, Soerjomataram I, Bray F (2018). Global Cancer Observatory: Cancer Today. Lyon, France: International Agency for Research on Cancer.[Internet]. Available from: https://gco.iarc.fr/today, accessed [Accessed 2018 Oct 11]
- Sankaranarayanan R, Swaminathan R, Brenner H, Chen K, Chia KS, Chen JG, et al. Cancer survival in Africa, Asia, and Central America: a population-based study. Lancet Oncol. 2010 Feb;11(2):165-73.
- Nessa A, Hussain MA, Rahman JN, Rashid MH, Muwonge R and Sankaranarayanan R. Screening for cervical neoplasia in Bangladesh using visual inspection with acetic acid. Int J Gynaecol Obstet, 2010;111:115-8.
- Basu P, Nessa A, Majid M, et al (2010). Evaluation of the National Cervical Cancer Screening Programme of Bangladesh and the formulation of quality assurance guidelines. J Fam Plann Reprod Helth Care, 2010;36:131-4.
- Ahmed T, Ashrafunnessa, Rahman J. Development of a Visual Inspection Programme for Cervical Cancer Prevention in Bangladesh. Elsevier Reproductive Health Matters, 2008;16:78-85.
- Strategic framework for the Comprehensive Control of Cancer Cervix in South-East Asia Region. World Health Organization 2015
- Nessa A, Rashid MH, Ferdous NE Chowdhury A. Screening for and management of high-grade cervical intraepithelial neoplasia in Bangladesh: A cross-sectional study comparing two protocols. J Obstet Gynaecol Res, 2013;39:564-71.
- Holme F, Kapambwe S, Nessa A, Partha B, Murillo R, Jeronimo J. Scaling up proven innovative cervical cancer screening strategies: Challenges and opportunities in implementation at the population level in low and lower-middle income countries. Int J Gynecol Obstet 2017;138 (Suppl. 1):63–68
- Nessa A, Naud P, Esmy PO, Joshi S, Rema P, Wesley R, Kamal M, Sauvaget C, Muwonge R, Sankaranarayanan Efficacy, Safety and Acceptability of Thermal Coagulation to Treat Cervical Intraepithelial Neoplasia: Pooled Data From Bangladesh, Brazil and India. Clin Gynecol Obstet. 2017; 6(3-4): 58-64
- Heath Bulletin, MIS, Directorate General of Health Services, Dhaka, Bangladesh, 2018; Preliminary Pre-Print Version.
- World Health Organization, WHO Guidelines for Screening and Treatment of Precancerous Lesions for Cervical Cancer Prevention, World Health Organization, Geneva, 2013.
- World health organization, Comprehensive Cervical Cancer Control: A guide to essential practice, Second edition. World health organization, Geneva 2014
- National Strategy for Cervical Cancer Prevention & Control Bangladesh (2017-2022), DGHS 2018.