Review Article
Is Histopathological Examination Essential for the Diagnosis of Psoriasiform Dermatitis?
*Kabir AN,1 Rahman MM 2
- *Dr. AKM Nurul Kabir, Associate Professor, Department of Pathology, Bangabandhu Sheikh Mujib Medical University, Dhaka, Bangladesh. kabir56@gmail.com
- Mohammad Mosiur Rahman, Assistant Professor, Department of Pathology, Bangabandhu Sheikh Mujib Medical University, Dhaka, Bangladesh
*For correspondence
Abstract
Psoriasiform dermatitis encompasses a wide range of diseases, some of which show both clinical and histological overlap. Psoriasis is generally thought to be a genetic disease that is triggered by environmental factors. Psoriasis is characterized by an abnormally excessive and rapid growth of the epidermal layer of the skin. Abnormal production and an over abundance of skin cells result from the sequence of pathological events in psoriasis, can be shown as a higher Ki-67 index compared with normal appearing, non-lesional skin. Morphometric analysis of histological features can also give a quantitative dimension to histopathology in diagnosis of psoriasis and in differentiating from other psoriasiform dermatitis. Psoriasis is also regarded as a T-cell mediated disorder, mainly CD4+ (helper/inducer) lymphocytes along with CD8+ subsets are known to occur. The patient often prove to be a diagnostic dilemma for both dermatologists and pathologists alike. However, clinical features when considered alone may not be reliable, as they vary with both disease duration and treatment. Though to give a precise diagnosis one relies on clinical correlation, histopathology is essential as it is possible to assign specific diagnosis in most cases with a logical and systematic histopathological approach. Morphometry along with the help of Ki-67 & Cyclin D1 and other immunostains of keratinocytes, and immunophenotyping of T-cell infiltrate, a definitive diagnosis can be made.
[Journal of Histopathology and Cytopathology, 2019 Jul; 3 (2):151-161]
Key words: Psoriasis, Psoriasiform dermatitis, Morphometry, Ki-67, CD4+, CD8+
Introduction
Psoriasiform dermatitis encompasses a wide range of inflammatory dermatoses, some of which show both clinical and histological overlap. The term psoriasiform means that the lesion either clinically or histopathologically mimic psoriasis and this group includes: psoriasis- the prototype of psoriasiform dermatitis,1 and others as seborrheic dermatitis, pityriasis rubra pilaris (PRP), allergic dermatitis, atopic dermatitis , nummular dermatitis, lichen simplex chronicus (LSC), prurigo nodularis, pityriasis rosea (PR), inflammatory linear verrucous epidermal nevus (ILVEN) and mycosis fungoides (MF). Besides, clinical features in one patient may differ at different times and the diagnosis get obscured.3 As there is varied clinical presentation, a definitive histopathological diagnosis is essential in the treatment of such inflammatory dermatoses.1 It is a challenging task even to experienced pathologists to give a precise diagnosis every time and one relies also on clinical correlation. However, a stepwise systematic histopathological approach enables one to reach at a specific diagnosis in most cases.2
The morphometry parameters such as length of rete ridges, the length of dermal papillae and the ratio of length/average width of rete redges are statistically significant in the differentiating psoriasis from psoriasiform dermatitis and can be used in addition to routine histopathology.3 As the prototype of psoriasiform dermatitis, psoriasis is a hyperproliferative skin disorder with increased epidermal turnover rate and mitotic index, proliferation markers Ki-67 & Cyclin D1 immunostain of keratinocytes can be added as diagnostic tools to differentiate from other non- psoriasiform dermatitis.4 Expression levels of pRb and p53 were found to be higher in the psoriasis group in a study, compared with the normal epidermis.5 Psoriasis is an autoimmune skin disease and regarded to be T- cell mediated disorder. CD4+ T-cells are important in initiating and maintaining the pathogenic process of psoriasis but cross-primed CD8+ T-cells are the main effector cells. Mixtures of CD4+ T cells and CD8+ T-cells are found in papillary dermis and epidermis of psoriatic lesion. Psoriasiform lesions on the other hand show a high proportion of CD4+ T-cells in dermis. Immunophenotyping of T-cell infiltrate in the lesion can be done in differentiating the cases.6
History of Psoriasis
History of psoriasis begins in Ancient Greece, when psoriasis, leprosy, and other inflammatory skin disorders were believed to be the same condition and the Greeks termed the skin diseases as psora, lepra and lichen. Psora referred to itch, and lepra from lopos & lepo (the epidermis & to scale respectively). Hippocrates (460-377 BC) used the word lopoi to describe the dry, scaly, disfiguring disorders. The Old Testament also lumped together many cutaneous disorders, including leprosy and psoriasis, by the biblical term tsaraat or zaraath. Lepers were considered divinely punished, and cruelty was imposed upon those who were suffered from psoriasis and leprosy alike. Roman medical writer Celsus (25BC-45AD) first described papulosquamous diseases, suggesting as psoriasis one of these. Galen (133-200) first used the term psoriasis, but his description was likely represented seborrheic dermatitis. Gilbert (1797-1866) and Hebra finally distinguished the clinical picture of psoriasis from that of leprosy.7
Epidemiology
Although psoriasis occurs worldwide, it is a common chronic inflammatory skin disorders affecting 1.5-2% population in the western countries and 1.3% in general population.6 The prevalence of psoriasis is low in certain ethnic groups such as the Japanese.8
Psoriasis can present at any age and has been reported at birth and in older people of advanced age. A bimodal age of onset has been recognized in several large studies. The mean age of onset for the first presentation of psoriasis can range from 15 to 20 years of age, with a second peak occurring at 55–60 years. Henseler and Christophers studied a series of 2147 patients and also reported as two clinical presentations of psoriasis, type I and II. Type 1 begins on or before age 40 years; Type II begins after the age of 40 years. Type I disease accounts for more than 75% of cases. Patients with early onset, tended to have more relatives affected and more severe disease than patients who have type II psoriasis. In addition, strong associations have been reported with human leukocyte antigen (HLA)-Cw6 in patients with early onset of psoriasis. The course and progress of psoriasis is unpredictable. In one study, 39% of patients reported complete remission of disease at the age between one and 54 years. Higher figures have been reported in Japan.8 A family history of the disease is common. Approximately 30% of patients have a first-degree relative with psoriasis, and the risk of psoriasis increases with the number of affected relatives a patient has.9
Lifestyle and Morbidity
There is a link between cigarette smoking and psoriasis severity. There is sufficient evidence that aggravation of psoriasis is associated with alcohol consumption. Various recent studies report association of diabetes and other cardiovascular diseases to the severe form of psoriasis.10 Recent research suggests that patients with psoriasis have a systemic inflammatory state, putting them at increased risk of cardiovascular complications, including metabolic syndrome, peripheral vascular disease, stroke, myocardial infarction, and cardiac death.11 Psoriasis is increasingly being recognized as a disease that not only affects the skin but also has multi-systemic implications. Increasing epidemiological evidence suggests that patients with psoriasis may be more obese compared with the general population. Although the exact mechanism underlying the epidemiological association between psoriasis and obesity is uncertain, researchers have theorized that adipocyte elaboration of pro-inflammatory cytokines may exacerbate psoriasis.12 Many, but not all, studies have shown a positive association between metabolic syndrome and cardiovascular disease (CVD) and psoriasis, especially for (young) patients with moderate to severe disease. A recent study showed that Glyc A, which is a novel biomarker for systemic inflammation was associated with psoriasis.13 Nearly 60% of psoriasis patients and 40% of psoriatic arthritis patients report their disease as a large problem in their everyday life. Psychosocial limitations of both diseases include enduring low self-esteem, feeling physically unattractive or sexually undesirable and avoiding social activities.14
Etiology
Etiology of psoriasis remains unknown, even though, it is believed to be multifactorial with numerous key components including genetic susceptibility, environmental triggers in combination with skin barrier disruption and immune dysfunction.15 Various data suggest that infection is an important trigger for psoriasis. Streptococcal throat infection can initiate and exacerbate chronic psoriasis.15 Another research has shown that the composition of the cutaneous microbiota is related to many dermatological diseases including psoriasis, atopic dermatitis, and acne vulgaris.16
Genetic Factors
Epidemiological studies have demonstrated that psoriasis has an important genetic component, where the role of environmental triggers (e.g., stress, mechanical trauma and streptococcal infections) is well documented. Familial recurrence is also documented and disease concordance is higher in monozygotic than dizygotic twins. So, psoriasis is widely regarded as a multifactorial disorder caused by the interaction between inherited susceptibility alleles and environmental risk factors.17 The molecular genetic basis of psoriasis is complex, however, there are evidence that multiple genes are involved. Seven major psoriasis susceptibility loci have been reported and a major susceptibility locus for psoriasis is at 6p21, referred to as PSORS1 and is overrepresented in all populations tested. An association between psoriasis and other loci has also been reported on chromosomes 1p (PSORS7), 1q (PSORS4), 3q (PSORS5), 4q (PSORS3), 17q (PSORS2), and 19p (PSORS6). The strength of associations between such genes and susceptibility to psoriasis, apart from PSORS1, is variable, may relate, in part, to heterogeneity among different populations.8
Mechanism
Psoriasis is characterized by an abnormally excessive and rapid growth of the epidermal layer of the skin. Abnormal production of skin cells and an overabundance of skin cells result from the sequence of pathological events in psoriasis. Skin cells are replaced every 7 days in psoriasis rather than the usual about 53 days.18 Exclusive cellular “responsibility” for the induction and maintenance of psoriatic plaques has not been clearly defined. Increased proliferation of keratinocytes and endothelial cells in conjunction with APC/T cell/monocyte/macrophage inflammation leads to the distinct epidermal and vascular hyperplasia that is characteristic of lesional psoriatic skin.15 CD8+ T cells seem to be dominant in the epidermis whereas the CD4 + T cells predominant subset in the dermis. Activated CD4+ T cells produce a variety of cytokines including interleukin-2 (IL-2), TNFα and γINF. TNFα stimulating keratinocytes may produce IL -8, a potent T- lymphocyte and neutrophil chemoattractant and may involved in the formation of Munro microabscess. γINF is believed to play in important role in the initiation of psoriatic lesion.18 In individuals with a genetic predisposition, external stimuli such as trauma (known as Koebner phenomenon), infections, stress, drugs, and alcohol can all trigger an initial episode of psoriasis. This initial trigger activates the innate immune system (Figure 1). Complexes of the antimicrobial peptide LL-37 and host DNA/RNA, both released by keratinocytes after common epidermal damage, activate plasmacytoid dendritic cells (pDCs) to produce large amounts of type I IFNs (α/β). Subsequently, type I IFNs trigger maturation and differentiation of dermal dendritic cells (dDCs), and these dDCs then stimulate autoreactive T cells. Thereby, psoriatic autoimmune T cells are biased to produce Th1 and Th17/Th22 cells and which induce TNFα,/INFγ and IL-17/IL-22 production respectively. These mediators act on keratinocytes, leading to the activation and proliferation. In addition, type I IFNs directly upregulate IL-22 receptor (IL-22R) on keratinocytes, increasing their responsiveness to IL-22, and inhibits terminal differentiation and induces hyperproliferation of keratinocytes leading to epidermal hyperplasia, resulting psoriasis.19 In psoriasis , along with epidermal changes there is markedly increased dermal vascularity. The dermal vascular changes have been evaluated and shown to be due to change from arterial-type vessels to venules. The vascular changes may also precede the epidermal alterations, as shown in some studies.20

Clinical Features
Psoriasis is a papulosquamous disease with variable morphology, distribution, severity and course. Papulosquamous diseases are characterized by scaling papules and plaques.8 There are five clinical subtypes of psoriasis: vulgaris (plaque), guttate, pustular, inverse, and erythrodermic. The most common variant of psoriasis is plaque psoriasis, which includes approximately 85%–90% of psoriatic patients.15 The lesions are typically distributed symmetrically on the extensor surfaces of elbows, knees, and lumbosacral area and scalp. Psoriasis may also develop at the site of trauma, known as Koebner’s phenomenon. Guttate psoriasis has drop-shaped lesions. Inverse psoriasis forms red patches in skin folds. Pustular psoriasis presents as small non-infectious pus-filled blisters. Erythrodermic psoriasis involves widespread inflammation and exfoliation of the skin over most of the body surface. Psoriatic nail disease affects fingernails more commonly than toenails with small pits in the nail plate.8
Clinical Diagnosis
Psoriasis is a clinical diagnosis, and a skin biopsy is usually not necessary for a classic presentation of the disease.9 Diagnosis of psoriasis is usually based on the appearance of the skin. The characteristic lesions are sharply demarcated, scaly, erythematous plaques, papules, or patches on skin that may be pruritic and/or painful. They may be ovoid, round or irregular and often distributed symmetrically.9 Auspitz sign, named after Heinrich Auspitz, where there is pinpoint bleeding on removal of scales from the lesions of psoriasis. The test by which Auspitz sign is elicited by light tangential scratching with the edge of glass slide is called as Grattage test can be used as clinical tool.21
Microscopic Diagnosis
Histopathology is considered as a “gold standard” for the diagnosis of most dermatological conditions including psoriasis.21 Common histological features in psoriasis vulgaris are hyperkeratosis, parakeratosis, psoriasiform hyperplasia (Figure 2), Munro microabscess / spongioform pustule of Kogoj, thin suprapapillary plate, hypogranulosis, dilated capillaries in papillary dermis and dermal inflammation.1 However, other than Munro microabscess, spongioform pustule of Kogoj and dilated tortuous capillaries in papillary dermis, the remaining features , such as parakeratosis, psoriasiform hyperplasia can be seen also in chronic eczematous dermatitis, such as atopic dermatitis, nummular dermatitis or allergic contact dermatitis and appear to be “psoriasiform”.18 However, following a systematic approach one can reach at conclusive diagnosis.

Tirumalae described a detail microscopic description for definitive diagnosis as follows.2
Scanning magnification
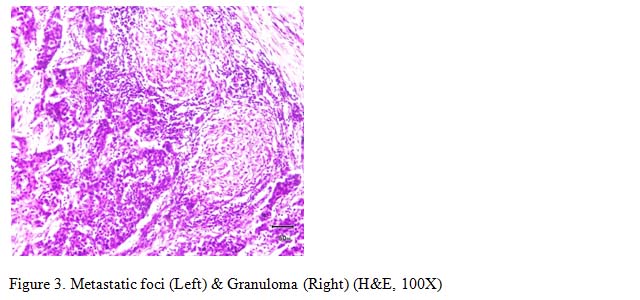
Examination of microscopic sections under scanning magnification forms the first step. The presence of evenly elongated, thin rete ridges with equally long dermal papillae can seen in one condition i.e., psoriasis. All other diseases exhibit an uneven psoriasiform pattern, where rete ridges are of uneven of lengths and thickness with thick supra-papillary plates as in PRP (Figure 3).
Stratum corneum
The normal basket-weave pattern is lost in most cases and it is common to find parakeratosis. Parakeratosis can be present in small mounds or may be broad and confluent. Mounds of parakeratosis can be present throughout the epidermis in conditions like psoriasis and dermatophytosis, in seborrheic dermatitis confined to the infundibular ostia or seen in both locations in PRP. The classic “checkerboard” pattern i.e., parakeratosis staggered in both vertical and horizontal fronts is seen in PRP. Confluent parakeratosis is seen in dermatophytosis, syphilis, pityriasis lichenoides chronica (PLC) and most importantly, in MF. A sharply defined thick zone of parakeratosis alternating with orthokeratosis and mild papillomatosis are features of ILVEN.
Epidermis
Diminished or absent granular layer is seen in classic psoriasis, but is not a constant feature. Significant amounts of plasma in the scale crust goes against a diagnosis of psoriasis, and large amounts of plasma and a rapidly proliferating epidermis are hostile to fungi. The finding of spongiotic vesicles in a psoriasiform dermatitis are seen in allergic contact/nummular dermatitis and seborrheic dermatitis. Spongiotic psoriasiform pattern is also encountered in patch-stage of MF.
Changes in Papillary Dermis
Psoriasis is characterized by thin supra-papillary plates and elongated dermal papillae with dilated, tortuous capillaries. The presence of extravasated erythrocytes is a sign of acuteness and is seen in eruptive psoriasis and PR. Vertical streaks of collagen with uneven psoriasiform acanthosis and compact orthokeratosis is diagnostic of LSC. However, changes of LSC can be superimposed on any chronic, itchy dermatitis including psoriasis. In contrast, thin haphazard, wiry bundles of collagen are seen in the papillary dermis in PLC and MF.
Nature of Infiltrate
Most of the psoriasiform dermatoses are dominated by lymphocytes in the dermis. When eosinophils are present among them, it indicates allergic/contact dermatitis or a drug eruption. However, eosinophils are not a pre-requisite for diagnosis of either of these conditions. Histiocytes and plasma cells in a psoriasiform dermatitis with scale crusts give hints for secondary syphilis. Superficial and deep infiltrates are seen in syphilis and lichen striatus (LS). In LS, there is a psoriasiform lichenoid pattern with deep infiltrates of lymphocytes along the adnexae, especially around the eccrine glands.
Morphometry
Morphometric analysis of histological features can give a quantitative dimension to histopathology. The results of morphometry parameters such as length of rete pegs, the length of dermal papillae and the ratio of length/average width of rete pegs can help in achieving the accurate diagnoses of psoriasis and psoriasiform dermatitis. In one study using eye-piece micrometer with the light microscope without special software and found statistically significant results in differentiating psoriasis from psoriasiform dermatitis. The mean length of rete pegs was 1.74 times greater in psoriasis when compared to psoriasiform dermatitis. The ratio of average length and width of rete pegs was considered representative of shape of rete pegs. The higher ratio of length over average width of rete pegs confirms the histopathological finding of slender long rete pegs, which favors the diagnosis of psoriasis.
The dermal vascular changes have been evaluated in different studies by electron microscopy and shown to be due to change from arterial-type vessels to venules. The vascular changes may also precede the epidermal alterations, as shown in some studies. Morphometric parameters of papillary dermal vessels in psoriasis and to compare these with psoriasiform lesions can also be used. Morphometric evaluation of dermal vasculature in psoriasis has shown increased endothelial and luminal volume of vessels compared to control subjects. On light microscopic evaluation of CD34 immunostained sections, biopsies from psoriasis showed much greater microvascular staining in the papillary dermis in comparison to psoriasiform dermatitis.20
Role of Immunohistochemistry
Ki-67 and Cyclin D1 Immunostaining
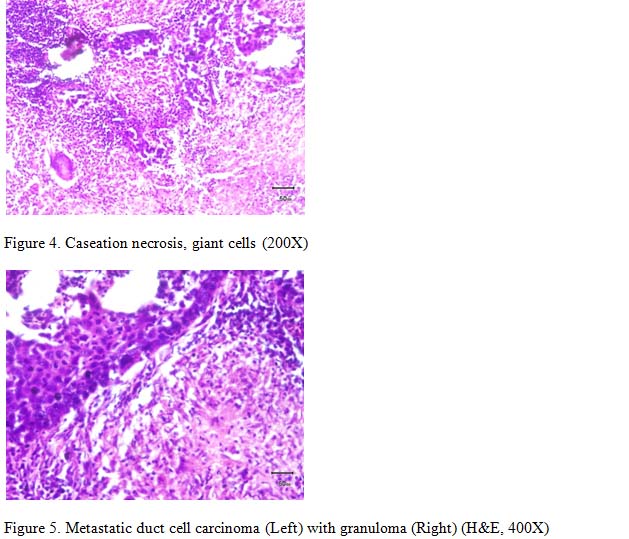
As Psoriasis is a hyperproliferative skin disorder with increased epidermal turnover rate and mitotic index, proliferation markers Ki-67 (Figure 4) and Cyclin D1 immunostaining can be used to differentiate psoriasis from non-psoraisis psoriasiform dermatitis( NPPD ) (Figure 5). In a study Ki-67 and Cyclin D1 positive cells were counted per mm2 of suprabasal and total epidermal area by Sezer. et al. 4

Psoriatic lesions have been shown to reveal a higher Ki-67 index compared with normal appearing, non-lesional skin. In psoriasis group, suprabasal Ki-67 positive cells were more than 75% of the total epidermal Ki-67 positive cells in the epidermis (including basal and suprabasal cell population) in psoriasis group, whereas this ratio was lower than 75% (cut-off value) in NPPD group. The suprabasal/total epidermal count ratio for Cyclin D1 immunostaining was higher in the psoriasis group compared with the NPPD group, but a cut-off value to distinguish between these two was not detected, suggesting that Ki-67 is a more sensitive marker than Cyclin D1 in terms of the presence of a cut-off value and could be a useful tool for dermatopathologists to differentiate psoriasis from other psoriasiform dermatitis.4
pRb and p53 Immunostaining
Expression levels of pRb and p53 were found to be higher in the psoriasis group in a study, compared with the normal epidermis. The phosphorylation of pRb is associated with cyclin D1, cyclin E and P16. pRb phosphorylation in psoriasis is incresed by the activity of cyclin D1 and Cyclin E and showed a higher expression of pRb than that of normal epidermal expressions. Total basal layer cell counts for p53 expression were found to be significantly higher in psorisis group compared with the normal group.5 It is postulated that increased expression of p53 in psoriatic skin is a physiological reaction indicating the attempt to counteract the proliferation and to repair DNA errors, and is most often expressed as an increased number of mitoses.22
CD4+ and CD8+ cell distribution
Psoriasis also known as a skin disorder with immunological factors playing an important role in its pathogenesis, and lymphocytic infiltrates, mainly CD4+ and CD8+ cells provide a major contribution in the initiation and maintenance of the lesion. Psoriasis is an autoimmune skin disease characterized by T-cell mediated hyperproliferation of keratinocytes. It is regarded as a T-cell mediated disorder, mainly CD4+ (helper/inducer) lymphocytes along with CD8+ (suppressor/cytotoxic) subsets are known to be associated. T-lymphocytes in psoriatic lesion are in an activated state with expression of HLA-DR and IL-2 receptor. Mixtures of CD4+ T-cells and CD 8+ T-cells are present in papillary dermis and epidermis of psoriatic lesion. T-cell also plays a role in the pathogenesis of psoriasiform lesions, and reported a high proportion of CD4+ T-cells in the dermis on immunohistochemical analysis.6
A comparative study was done by Rana. et al to see the infiltration of CD4+ and CD8+ cells in psoriasis and psoriasiform lesions. The inflammation in the epidermis was present in about half of psoriasis cases and predominant cells were polymorphs. In the upper dermis, inflammation was evident in all cases with predominant cells were lymphocytes. Inflammation in the lower (reticular) dermis was present with mostly lymphocytes.
In psoriasiform lesions the inflammation was present in the epidermis in only few cases showing mixtures of polymorphs and lymphocytes. Within the upper dermis, all cases showed inflammation with predominant of lymphocytes. Few cases showed inflammation in the lower dermis with lymphocytes as majority of the cells. Immunohistochemical staining was done to see the distribution of CD4+ and CD8+ cells. the distribution of CD4 positive cells was seen in psoriasis patients. In the epidermis of psoriasis cases only one fifth were positive for CD4+ cells. In the upper dermis, CD4+ cells were present in 92% cases. In the lower dermis about half of cases were positive for CD4+ cells.
D 8+ positive cells on the other hand were seen in the epidermis in 40% cases. In the upper dermis, all the cases showed CD8+ positive cells. In the lower dermis, CD8+ positive cells were found in large number of cases.
An immunophenotyping of the inflammation of psoriasiform lesions showing, CD4+ cells as predominant cells in the upper dermis. In lower dermis area showed 16% cases having CD4+ cells.
Various studies have shown that CD4+ cells are less frequent in psoriatic epidermis. In epidermis CD8+ cells were seen in 40% cases, and 8% in psoriasiform lesions. The difference was statistically significant. In the upper dermis, one study has shown the mixtures of CD4+ and CD8+ T-cells in psoriasis, whereas psoriasiform group showed that CD4+ cells in abundance.
The difference in amount and pattern of CD4+ and CD8+ T-cells in the various compartments is helpful in differentiating between psoriasis and psoriasiform lesions especially in cases with borderline morphology.6
Conclusion
Psoriasis, the prototype of psoriasiform dermatitis, is a genetically determined, inflammatory, and proliferative disease of the skin characterized by dull red, sharply demarcated scaly plaques. The two clinical signs, Auspitzs sign and the Grattage test have been described as pathognomonic of psoriasis when biopsy is not done. However, these signs are present only in untreated patients. Psoriasis has many different clinical differentials as other psoriasiform lesions. Besides, the same patient can present at different times with a different clinical presentation. Since satisfactory management of the condition requires both symptomatic and specific therapy, it is essential to reach a definitive diagnosis. The recurrent nature and prognosis of psoriasis differs from that of psoriasiform dermatitis, thus, further highlighting the importance of reaching the correct diagnosis. Clinical features, considered alone, may not be reliable. Histopathology is regarded as a gold standard for the diagnosis of most dermatological conditions including psoriasis and constitutes definite hard evidence, which can be preserved for future review. Though to give a precise diagnosis one relies on clinical correlation, histopathology is essential as it is possible to assign specific diagnosis in most cases with a logical and systematic histopathological approach. In selected cases morphometry, Ki-67 & Cyklin D1, pRb and p53 immunostaining of keratinocytes can be added when needed. The pattern of T-cell infiltrate by immunophenotyping can give an additional diagnostic clue.
Acknowledgement
The authors are grateful to Faisal Kabir Taj for his help in preparing the figure 1.
References
- Jayalakshmy PL, Babitha AM, Sankar S, Nandakumar G. Histopathological spectrum of Psoriasiform dermatitis. Journal of Pathology of Nepal 2016; 6(12): 975 -980.
- Tirumalae R . PsoriasiformDermatoses: Microscopic Approach,Indian J Dermatol. 2013 58(4): 290–293. doi: 4103/0019-5154.113945.
- Shirish S. Chanadanwale, Narayanan K. Panicker, Sushmah P. Kulkarni, Komal R. Shah, Kumar H, Yugal K. Sharma1, Sukanya Pal, Morphometry analysis of psoriasis and psoriasiform dermatitis: A retrospective study of 50 cases. Medical Journal of D.Y. Patil University 2015; 8(1): 43-47.
- Sezer E, Böer-Auer A, Cetin E, Tokat F, Durmaz E, Sahin S and Ince U. Diagnostic utility of Ki-67 and Cyclin D1 immunostaining in differentiation of psoriasis vs. other psoriasiform dermatitis. Dermatol Pract Concept. 2015;5(3): 7-13. 2015;5(3):2ul; 5(3):doi: 5826/dpc.0503a02.
- Kim SA, Ryu Y W, Kown J I, Choe M S, Jung J W, Cho J W. Differential expression of cyclin D1, Ki‑67, pRb, and p53 in psoriatic skin lesions and normal skin. MolecularMedicine Reports 2018;17: 735-742, DOI: 10.3892/mmr.2017.8015.
- Rana S, Zeeba J S, Sujata J, Madhur K: A comparative study of psoriasis and psoriasiform lesion on basis of CD4 and CD8 cell infiltration. Our Dermatol Online. 2012; 3(4): 292-297.
- Cowden A., Van Voorhees A.S. (2008) Introduction: History of psoriasis and psoriasis therapy. In: Weinberg J.M. (eds) Treatment of Psoriasis. Milestones in Drug Therapy. Birkhäuser Basel, pp 1-2. DOIhttps: doi.org/10.1007/978-3-7643-7724-3_1.
- Langley R G B, Krueger G G, Griffiths C E M, Psoriasis: Epidemiology, Clinical Features, and Quality of Life. Ann Rheum Dis. 2005;64(Suppl II):ii18 23.doi: 10.1136/ard.2004.033217.
- Grace W. Kimmel and Mark Lebwohl. Psoriasis: Overview and Diagnosis.Bhutani T et al. (eds.), Evidence-Based Psoriasis, Upsoriasiformdermatitisates in Clinical Dermatology, https://doi.org/10.1007/978-3-319-90107-7_1.
- Khan ZA, Malik LM, Jahangir M, Prevalence of smoking, alcohol, and comorbid conditions in psoriasis. Journal of Pakistan Association of Dermatologists 2010; 20:212-216.
- Sako E, Famenini S, Jashin J Wu. Trends in Type of Original Psoriasis Publications by Decade, 1960 to 2010. Perm J 2016 Fall;20(4):15-060. http://dx.doi.org/10.7812/TPP/15-060.
- Armstrong AW, Harskamp CT, Armstrong EJ. The association between psoriasis and obesity: a systematic review and meta-analysis of observational studies. Nutrition and Diabetes (2012) 2, e54; doi:10.1038/nutd.2012.26..
- Samuel T. Hwang, Nijsten T and Elder J T. Recent Highlights in Psoriasis ResearchJournal of Investigative Dermatology 2017; 137(3):550 -556; doi:10.1016/j.jid.2016.11.007.
- Busse K, Liao W.Which Psoriasis Patients Develop Psoriatic Arthritis? Psoriasis Forum. 2010; 16(4): 17–25.
- Ayala-Fontánez N, Soler D C, McCormick TS. Current Knowledge on Psoriasis and Autoimmune Diseases. Psoriasis: Targets and Therapy 2016;6: 7–32;.org/10.2147/PTT.S64950.
- Benhadou F, Mintoff D, Schnebert B, Thio H B. Psoriasis and Microbiota: A Systematic Review. Diseases 2018, 6, 47; doi:10.3390/diseases6020047.
- Capon F. The Genetic Basis of Psoriasis. Int J Mol Sci. 2017;18(12):2526. Published 2017 Nov 25. doi:10.3390/ijms18122526.
- Mobini N, Toussaint S, Kamino H: Noninfectious Erythematous, Papular, and Squamous diseases. In Lever’s Histopathology of the Skin, 10 th Edition. Edited by Elder DE, Elenitsas R, Johnson BL, Murphy GF, Xu X. India, Woltrs Kluwer, 2009, pp 169-203.
- Flatz L, Conrad C. T-cell-mediated inflammation in psoriasis: pathogenesis and targeted therapy.Psoriasis: Targets and Therapy 2013; 3:1-10. org/10.2147/PTT.S26339.
- GuptaS, KaurM, Gupta R, SinghS, PantL, SinghP P.Dermal Vasculture in Psoriasis and Psoriasiform dermatitis: a Morphometric study. Indian J Dermatol. 2011 Nov-Dec; 56(6): 647–649. doi: 10.4103/0019-5154.91820: 10.4103/0019-5154.91820
- Mehta S, Singal A, Bhattacharya SN. A study of clinicohistopathological correlation in patients of psoriasis and psoriasiform dermatitis. Indian J Dermatol Venereol Leprol 2009;75:100.
- Baran W, Szepietowski J. C, Szybejko-Machaj G. Expression of p53 protein in psoriasis. Acta Dermatoven APA 2005;14(3):79-83.