Imprint Cytology in the Diagnosis of Upper Gastrointestinal Lesions
*Keya SA,1 Saha NK,2 Alam MJ,3 Ullah P,4 Shariar S,5 Hira AD,6 Ahmed NU,7 Islam N8
Abstract
Endoscopic biopsy and cytology are well established techniques for the diagnosis of upper gastrointestinal tract malignances. Imprint cytology is a touch smear preparation which helps to diagnose malignant cell easily. This cross sectional study was done to see imprint cytological patterns of benign and malignant lesions of upper gastrointestinal tract, to find out histopathological diagnoses and to compare imprint cytological diagnoses with histopathological diagnoses. Biopsy materials from 100 patients were obtained by endoscopist using video endoscope and were subjected to imprint smear technique followed by histopathological examination of the same materials. Cytological and histopathological diagnoses were compared using appropriate statistical methods. Among the 100 cases, 57(57%) were male & 43(43%) were female with a mean age of 56.7 years. Out of 100 cases, gastric, esophageal and duodenal lesions were 63(63%), 32(32%) and 5(5%) respectively. Misinterpretation on cytological evaluation was seen in only 6 cases. The overall sensitivity, specificity, positive predictive value, negative predictive value and diagnostic accuracy of imprint cytology were 98.46%, 91.42%, 95.52%, 96.97% and 96% respectively. The findings of the present study indicate that imprint cytological method is a reliable technique for rapid diagnosis of upper GIT lesions as it is simple, accurate and cost effective. Diagnosis can be provided within an hour of endoscopic procedure by the imprint smear technique.
[Journal of Histopathology and Cytopathology, 2018 Jan; 2 (1):23-29]
Keywords: Imprint cytology, Upper Gastrointestinal Lesions
- *Dr. Shamim Ara Keya, Lecturer of Pathology, Shaheed Suhrawardy Medical College, Dhaka. keyaparash@gmail.com
- Professor Dr. Naba Kumar Saha, Professor and Head, Department of Pathology, Sylhet MAG Osmani Medical College, Sylhet.
- Md. Jahangir Alam, Associate Professor and Head, Department of Gastroenterology, Sylhet MAG Osmani Medical College, Sylhet.
- Parash Ullah, Medical Officer, Department of Medicine, Shaheed Suhrawardy Medical College Hospital, Dhaka.
- Sakib Shariar, Pathologist, Bangladesh Railway Hospital, Chittagong.
- Ananda Dyuti Hira, Pathologist, Khulna Medical College, Khulna.
- Nasir Uddin Ahmed, Pathologist, Faridpur Medical College, Faridpur.
- Nazmul Islam, Assistant Professor of Pathology, Army Medical College, Comilla.
*For correspondence
Introduction
Any portion of the gastrointestinal tract may be affected by malignancy. The highest incidence of malignancy is in the esophagus, stomach and colorectal region. In fact esophagogastric and colorectal malignancies are amongst the commonest cancers in humans.1 Worldwide, gastric adenocarcinoma is the second most common cancer.2 Endoscopic biopsy and cytology are well established techniques for the diagnosis of upper gastrointestinal tract malignancies. Now a days, various cytologic techniques like brush cytology, crush preparation, touch smear or imprint cytology are commonly used along with routine endoscopic biopsy.3
Imprint cytology from endoscopic biopsy is highly sensitive and specific technique for the diagnosis of upper GI malignancy. Imprint cytology showed an overall accuracy of 97.6%, 100% and 100% for the diagnosis of malignancies of esophagus, stomach and duodenum respectively.4 But there is no systemic study on imprint cytology of gastrointestinal lesions in our country. Imprint cytology can act as an adjunct to histopathology as it increases the diagnostic efficacy and saves time but definitely it cannot replace histopathology as chances of false positives are high.5 Imprint cytology is a special variation of applied cytology that can be used for various purposes.6 Sometimes endoscopic biopsy fails to make a definitive histological diagnosis due to inadequate tissue from small lesion where tissues are distorted during histological processing; in that case imprint cytology may be useful in diagnosing upper gastrointestinal tract malignancy.7 In this study, imprint smears were taken before keeping the endoscopic specimens in fixative for histopathological examination. Endoscopic biopsy is an essential part of the evaluation of gastrointestinal pathology. In the diagnosis of upper GI lesions, histopathological examination is considered gold standard but is time-consuming when compared to cytology. Most gastroenterologists and patients would like to get an immediate opinion regarding the adequacy of biopsy and nature of the lesion. Imprint cytology is a simple, rapid, reliable and cost effective method and it alone can serve as a useful tool for an immediate diagnosis within an hour after endoscopic procedure. Imprint cytology lets the surgeon to plan a therapeutic strategy approximately one week earlier.4,8 With this background, this study was designed to find out imprint cytological patterns of benign and malignant lesions of upper gastrointestinal tract, to find out histopathological diagnoses and to compare imprint cytological diagnoses with histopathological diagnoses.
Methods
This study was a cross sectional study and carried out on 100 patients in the department of Pathology, Sylhet MAG Osmani Medical College, Sylhet in collaboration with the department of Gastroenterology, Sylhet MAG Osmani Medical College Hospital, Sylhet, Bangladesh from 1st January 2015 to 31st December 2015. During endoscopic examination by using video endoscope, biopsy was taken. Imprint smears were prepared from all biopsy samples. Imprint smear was done by placing tissue on the slides from the biopsy forcep with the help of a fine needle. After placing tissue on the slides, thin smears were prepared by gently rotating the tissue with the needle. Then smears were fixed in 95% ethyl alcohol and stained with Papanicolaou stain.The same tissue after smear preparation was collected for histopathological examination. The tissue was examined thoroughly in day light with particular emphasis on number, colour, consistency, presence or absence of hemorrhage and necrosis. Tissue was embedded as such and was placed in bottle containing 10% formalin with proper tagging and was kept for overnight fixation. Routine tissue processing with paraffin impregnation was done and sections were stained with haematoxylin and eosin. The diagnosis of upper gastrointestinal tract malignancy was done according to the cytopathological and histopathological findings and grading was done by WHO classification. Then imprint smear diagnosis was compared with the histopathological diagnosis. The efficacy of imprint cytology was determined by sensitivity, specificity, positive predictive value, negative predictive value and accuracy.
Results
Among the 100 patients, the age ranged from 21 to 100 years with a mean of 56.7 years. In this study, 57(57%) were male and 43(43%) were female with male to female ratio of 1.33:1. The highest number of patients 30(30%) was in the age group 61-70 years followed by 27(27%) in 41-50 years age group & 21(21%) in 51-60 years age group. In our study, 63% (63 cases) were located in the stomach, 32 % (32 cases) were in the esophagus, and 5% (5 cases) were in the duodenum. The most common presenting symptoms were pain and vomiting in case of gastric lesions and dysphagia in case of esophageal lesions.
Table I: Imprint cytology and corresponding histopathological diagnosis in contingency (cross) table
| Cytological diagnosis
|
No |
Histopathological diagnosis |
T
o
t
a
l |
||||||||||
| Adenocarcinoma | Squamous cell carcinoma | Chronic non atrophic gastritis | Suggestive of adenocarcinoma | Chronic gastric ulcer | Chronic duodenitis | Dysplasia | Suggestive of squamous cell carcinoma | Chronic esophagitis | Hyperplastic polyp | Gastric adenoma | |||
| Adenocarcinoma | 35 | 34 | 1 | 35 | |||||||||
| Squamous cell carcinoma | 25 | 25 | 25 | ||||||||||
| Chronic gastritis | 24 | 23 | 1 | 24 | |||||||||
| Suspicious of adenocarcinoma | 5 | 4 | 1 | 5 | |||||||||
| Chronic gastric ulcer | 3 | 3 | 3 | ||||||||||
| Suspicious of squamous cell carcinoma | 2 | 1 | 1 | 2 | |||||||||
| Chronic duodenitis | 2 | 2 | 2 | ||||||||||
| Normal findings | 2 | 1 | 1 | 2 | |||||||||
| Chronic esophagitis | 1 | 1 | 1 | ||||||||||
| Dysplasia | 1 | 1 | 1 | ||||||||||
| Total | 100 | 35 | 25 | 24 | 4 | 4 | 2 | 2 | 1 | 1 | 1 | 1 | 100 |
Ulcerative (41%) and ulceroproliferative lesions (41%) were the most common endoscopic findings. Proliferative lesion was found in 17% of cases and benign polyp was noted in 1% of cases. In the present study, the most common lesion diagnosed by imprint cytology was adenocarcinoma (35%) followed by squamous cell carcinoma (25%) and chronic gastritis (24%) (Table-1). Histopathological evaluation revealed that the most common tumor was adenocarcinoma (35%) followed by squamous cell carcinoma (25%), chronic non atrophic gastritis (24%), suggestive of adenocarcinoma (4%), chronic gastric ulcer (4%), chronic duodenitis (2%), dysplasia (2%) & suggestive of squamous cell carcinoma, chronic esophagitis, hyperplastic polyp, gastric adenoma 1 case each (Table I).
Complete correlation between imprint cytological and histopathological diagnosis was obtained in 94(94%) cases (Table II) and 6 cases were misinterpreted on cytological examination. Out of six misinterpreted cases, two cases were diagnosed as normal findings on imprint smears which were subsequently diagnosed as adenocarcinoma in one case and chronic gastric ulcer in another case on histopathology. One case was diagnosed as adenocarcinoma on imprint smears which was subsequently diagnosed as chronic non atrophic gastritis on histopathology. Another one case was diagnosed cytologically as chronic gastritis was diagnosed histologically as hyperplastic polyp. Cytological diagnosis of suspicious of squamous cell carcinoma in one case was confirmed as moderate dysplasia by histopathology. Cytologically one case was interpreted as suspicious of adenocarcinoma which was diagnosed as gastric adenoma on histopathological examination.
Table II: Correlation of histopathological and cytopathological diagnoses
| Histopathological diagnosis | No. of Cases | Cytological correct diagnosis | Percentage |
| Adenocarcinoma | 35 | 34 | 97.05 |
| Squamous cell carcinoma | 25 | 25 | 100 |
| Chronic nonatrophic gastritis | 24 | 23 | 95.83 |
| Suggestive of adenocarcinoma | 4 | 4 | 100 |
| Chronic gastric ulcer | 4 | 3 | 75 |
| Chronic duodenitis | 2 | 2 | 100 |
| Dysplasia | 2 | 1 | 50 |
| Suggestive of Squamous cell carcinoma | 1 | 1 | 100 |
| Chronic esophagitis | 1 | 1 | 100 |
| Hyperplastic polyp | 1 | 0 | 0 |
| Gastric adenoma | 1 | 0 | 0 |
| Total | 100 | 94 | 94 |
Statistical evaluation of imprint cytology was done (Table III) and validity of imprint cytology like sensitivity, specificity, PPV, NPV and accuracy were found as 98.46%, 91.42%, 95.52%, 96.97% and 96% respectively (Table IV).
Table III: Statistical evaluation of cytopathological diagnosis of 100 cases of upper GIT lesions
| Histopathological diagnosis | Cytopathological Diagnosis | ||||
| Disease positive (Malignant) | Disease negative(Benign) | ||||
| Positive(Malignant)
|
65
|
TP | 64 | FP | 3 |
| Negative(Benign)
|
35
|
FN | 1 | TN | 32 |
| Total | 100 | Total | 65 | Total | 35 |
TP= True positive, TN= True negative, FP= False positive, FN= False negative.
Table IV: Validity of cytopathological diagnosis of 100 cases of upper GIT lesions.
| Sensitivity | Specificity | PPV | NPV | Accuracy |
| 98.46% | 91.42% | 95.52% | 96.97% | 96% |
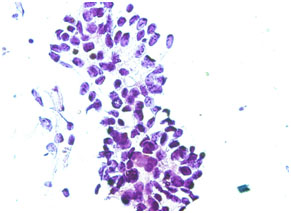
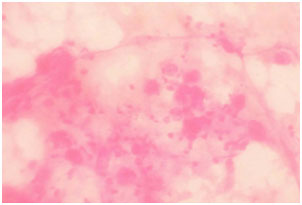
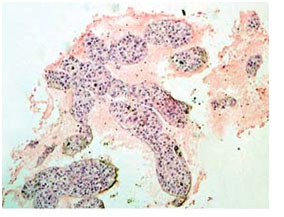
Figure 1. Photomicrograph of imprint cytology of adenocarcinoma (Papanicolaou stain, x40).
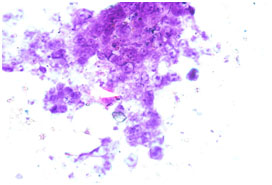
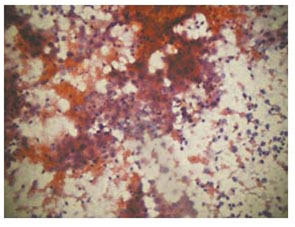
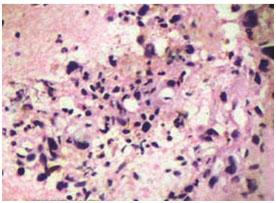
Figure 2. Photomicrograph of imprint cytology of squamous cell carcinoma (Papanicolaou stain, x40).
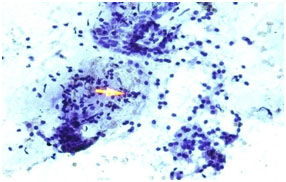
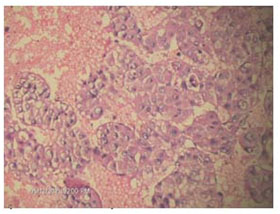
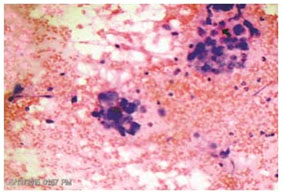
Figure 3. Photomicrograph imprint cytology of chronic gastritis (Papanicolaou’s stain, x40).
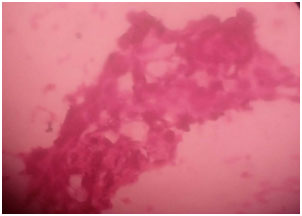
Figure 4. Photomicrograph of imprint cytology of gastric ulcer (Papanicolaou stain, x40).
Discussion
The primary role of gastrointestinal tract cytology is the detection of cancer. Gastrointestinal cytology is still in its early stages of development and few studies have described the role of brush cytology and imprint cytology in interpretation of upper GI biopsy.
The age of study patients ranged from 21 years to 100 years with a mean of 56.7 years. Of the 100 patients, 57(57%) were male and 43(43%) were female with male to female ratio of 1.33:1. This observation is similar to other studies who also observed that the frequency of gastrointestinal lesions was more in male.4,9 Highest number (30%) of gastrointestinal lesions were found in the age group 61 to 70 years followed by 27(27%) in 41 to 50 years age group and 21(21%) in the age group of 51 to 60 years which have consistence with the study of Vijayanarasimha D et al9 who observed highest number in fifth to seventh decades of life with a mean age of 55 years. In the present study, 63% lesions were in the stomach, 32% were in the esophagus and 5% were in the duodenum which are also close to the findings of the study done by Vijayanarasimha D et al9 who observed that out of 110 cases, 52(47.3%) were gastric, 45(40.9%) were esophageal and 13(11.8%) were duodenal lesions. The clinical presentations of study patients were upper abdominal or epigastric pain, dysphagia, vomiting, anorexia, distended abdomen and sometimes abdominal mass. Abdominal or epigastric pain was the commonest symptom in case of gastric and duodenal lesions and dysphagia in case of esophageal lesions. This clinical observation is similar to the clinical findings of the study done by Vijayanarasimha D et al.9 In our study, endoscopic findings of upper GIT lesion were ulcerative (41%), ulcero-proliferative (41%), proliferative (17%) and polypoid (1%). In this study, among 100 cases of upper GIT lesions, 65(65%) were malignant and 35(35%) were benign. Diagnostic accuracy of imprint cytology of esophageal, gastric and duodenal lesions were 96.88%, 95.24% and 100% respectively which corresponds to or even better than some of the other studies.4,5,9,10,11 Histopathological evaluation of biopsies from 100 cases revealed that the most common lesion was adenocarcinoma (35%) followed by squamous cell carcinoma(25%), chronic non atrophic gastritis (24%), suggestive of adenocarcinoma(4%), chronic gastric ulcer (4%), chronic duodenitis (2%) and dysplasia (2%). Chronic esophagitis, hyperplastic polyp, gastric adenoma constituted one case each.
Complete correlation between imprint cytological and histopathological diagnosis was obtained in 94(94%) cases and 6 cases were misinterpreted on cytological examination. One false negative case found in this study that was observed in gastric lesion. This false negative result may be due to subepithelial location of the lesion which was missed on imprint smear. False negative diagnosis in imprint cytology was also observed in subepithelial lesions studied by Asha M et al.10 On endoscopic examination, ulceroproliferative lesion was seen in two cases in the gastric antrum. In one case, imprint cytology smears showed anaplastic epithelial cells and a diagnosis of adenocarcinoma was made. Histopathological examination showed chronic non atrophic gastritis and did not reveal any evidence of malignancy. Other case was interpreted as suspicious of adenocarcinoma by imprint smear which was subsequently diagnosed as gastric adenoma with dysplastic change by histopathology. On endoscopic examination, an ulceroproliferative lesion was seen at the lower end of esophagus which was interpreted as suspicious of squamous cell carcinoma on imprint smear but histopathological examination revealed moderate dysplasia. In the present study, three false positive diagnoses were made by imprint cytology. False positive diagnosis was also reported by other researchers and they concluded that the false positive diagnosis was due to regenerative atypia.9,11
The highest correlation (100%) was observed between imprint cytology and histopathology in the diagnosis of squamous cell carcinoma, suggestive of adenocarcinoma, suggestive of squamous cell carcinoma, chronic duodenitis and chronic esophagitis.
The overall sensitivity, specificity, positive predictive value, negative predictive value and diagnostic accuracy of imprint cytology in the diagnosis of upper gastrointestinal lesions were 98.46%, 91.42%, 95.52%, 96.97% and 96% respectively which are similar to other studies.4,9
Conclusion
The findings of the present study indicate that imprint cytology is a reliable technique for rapid diagnosis of upper GIT lesions as it is simple, accurate and cost effective. Diagnosis can be provided within an hour of endoscopic procedure by the imprint smear technique. So, gastroenterologist or surgeon can take a therapeutic decision approximately one week earlier.
References
- Conrad R, Castelino-Prabhu S, Cobb C, Raza A. Role of cytopathology in the diagnosis and management of gastrointestinal tract cancers. Journal of Gastrointestinal Oncology 2012; 3: 285-98.
- Zhang XF, Huang CM, Lu HS et al. Surgical treatment and prognosis of gastric cancer in 2613 patients. World Journal of Gastroenterology 2004; 10: 3405-08.
- Batra M, Handa U, Mohan H, Sachdev A. A Comparison of cytohistologic techniques in diagnosis of gastroesophageal malignancy. Acta Cytologica 2008; 52: 77-82.
- Sanjeevreddy M, Kittur SK, Jakareddy RB, Patil SY, Yelikar BR. Role of imprint cytology in the diagnosis of upper gastrointestinal tract lesions. Indian Journal of Public Health Research and Development 2013; 4: 190-95.
- Sharma P, Misra V, Singh PV, Misra SP, Gupta SC. A correlative study of histology and imprint cytology in the diagnosis of gastrointestinal tract malignancies. Indian Journal of Pathology & Microbiology 1997;40:139-146.
- Muller HA. Imprint cytology, advantages and possibilities. Entrez Pub Med 1976; 94: 7-10. [Online]
- Lal N, Bhasin DK, Malik AK, Gupta NM, Singh K, Mehta SK. Optimal number of biopsy specimens in the diagnosis of ca esophagus. Gut 1992; 33: 724-26.
- Cubukçu A, Gönüllü NN, Kaçar SO, Alponat A, Paksoy N. Imprint cytology in the endoscopic diagnosis of gastrointestinal malignancies. Hepatogastroenterology 2002; 49: 198-200.
- Vijayanarasimha D, Mahadevappa A, Manjunath GV, Sunila R. Imprint cytology: A diagnostic aid in interpretation of upper gastrointestinal endoscopic biopsies. Journal of Digestive Endoscopy 2014; 5: 144-148.
- Asha M, Divya V, Manjunath GV, Sunila R. Application of imprint cytology in interpretation of esophageal biopsies. Journal of Evolution of Medical and Dental Sciences 2013; 2: 4350-7.
- Mysorekar VV, Dandekar CP, Satyaprakash BS, Sarkar A. Role of imprint cytology in the diagnosis of gastrointestinal tract malignancies. Indian Journal of Pathology & Microbiology 2003; 46: 37- 43.